Types of Bone Grafts and Membranes in Dental Implantology
Introduction
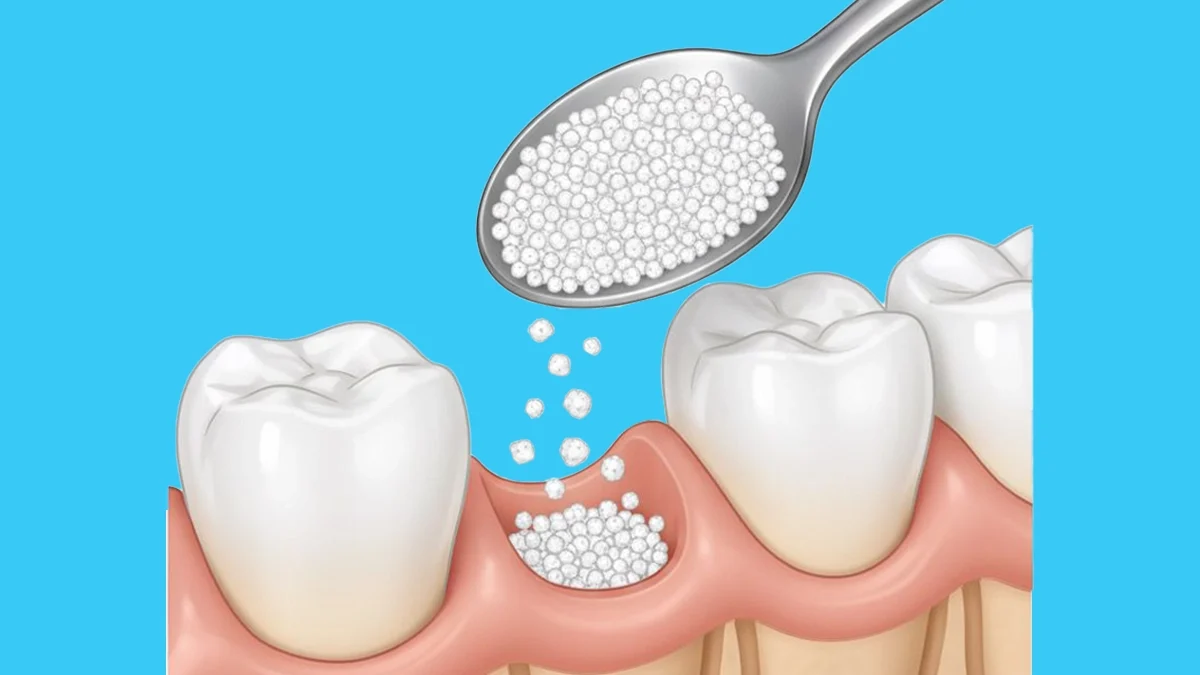
Successful implant placement depends on more than precision and technique — it relies on the quality and quantity of available bone. When alveolar bone is insufficient, bone grafting becomes essential to create a stable foundation for dental implants. Along with graft materials, barrier membranes play a crucial role in guiding tissue regeneration and preventing soft tissue invasion.
In this article, we will explore the different types of bone grafts and membranes, their clinical applications, and how they contribute to predictable implant success.
1-What Is Bone Grafting?
Bone grafting is a regenerative surgical procedure designed to replace or augment lost bone in the jaws. The goal is to restore the anatomical structure and provide adequate bone volume for implant stability. Grafting materials can either stimulate the body’s natural bone formation or act as scaffolds that are gradually replaced by new bone.
2-Types of Bone Grafts
a-Autograft (Autogenous Bone Graft)
- Source: Harvested from the patient’s own body — commonly from intraoral sites (chin, ramus, maxillary tuberosity) or extraoral sites (iliac crest).
- Advantages:
- Contains living cells and growth factors.
- High osteogenic, osteoinductive, and osteoconductive potential.
- No risk of immune reaction.
- Disadvantages:
- Limited quantity available.
- Requires a second surgical site, increasing morbidity.
Clinical use: Ideal for major defects, sinus lifts, and ridge augmentations where rapid integration is critical.
b-Allograft (Human Donor Bone)
- Source: Bone derived from another human, processed and sterilized in tissue banks.
- Types:
- Freeze-Dried Bone Allograft (FDBA) – mainly osteoconductive.
- Demineralized Freeze-Dried Bone Allograft (DFDBA) – contains bone morphogenetic proteins (BMPs) with osteoinductive potential.
- Advantages:
- No need for a donor site.
- Good biocompatibility.
- Disadvantages:
- Slower remodeling than autografts.
- Minimal risk of disease transmission (extremely low with modern processing).
Clinical use: Ridge preservation, sinus augmentation, and socket grafting.
c-Xenograft (Animal-Derived Bone)
- Source: Typically bovine or porcine bone that has been deproteinized and sterilized.
- Advantages:
- Excellent osteoconductive scaffold.
- Long resorption time maintains space for new bone formation.
- Widely available.
- Disadvantages:
- No osteogenic or osteoinductive properties.
- May remain partially unresorbed.
Clinical use: Commonly used for sinus lifts, ridge preservation, and peri-implant defects.
d-Alloplast (Synthetic Bone Substitutes)
- Source: Man-made materials such as hydroxyapatite (HA), β-tricalcium phosphate (β-TCP), or bioactive glass.
- Advantages:
- Unlimited availability.
- No risk of disease transmission.
- Resorption rate can be controlled by material composition.
- Disadvantages:
- Primarily osteoconductive — lacks biological activity.
Clinical use: Minor defects, socket preservation, and as a composite with autogenous or allograft materials.
e-Composite Grafts (Combination Grafts)
Combining different materials (e.g., autograft + xenograft) can optimize biological performance — blending osteogenic potential with long-term volume stability.
Clinical use: Complex ridge augmentations and sinus lifts requiring both rapid integration and volumetric stability.
3-Barrier Membranes in Guided Bone Regeneration (GBR)
Purpose of Membranes
In Guided Bone Regeneration (GBR), membranes act as barriers that prevent soft tissue from invading the bone graft area, allowing osteogenic cells to populate the defect and form new bone. The ideal membrane should be biocompatible, cell-occlusive, easy to handle, and maintain space during healing.
4-Types of Membranes
a-Resorbable Membranes
- Materials: Collagen (bovine or porcine origin), polylactic acid (PLA), or polyglycolic acid (PGA).
- Advantages:
- No need for second surgery to remove the membrane.
- Good handling and biocompatibility.
- Disadvantages:
- Limited space maintenance.
- Degradation time must match bone healing rate.
Clinical use: Ridge preservation, minor GBR, and extraction socket grafting.
b-Non-Resorbable Membranes
- Materials: Expanded Polytetrafluoroethylene (ePTFE), dense PTFE (dPTFE), or titanium-reinforced PTFE.
- Advantages:
- Excellent space maintenance.
- Suitable for large or complex defects.
- Disadvantages:
- Requires a second surgery for removal.
- Higher risk of exposure or infection if soft tissue dehiscence occurs.
Clinical use: Vertical and horizontal ridge augmentation, severe defect reconstruction.
c-Titanium Mesh and Titanium-Reinforced Membranes
- Purpose: Provide mechanical stability and maintain the shape of the grafted area.
- Advantages:
- Excellent space maintenance.
- Can be used with particulate grafts or block grafts.
- Disadvantages:
- Technique-sensitive; exposure risk if soft tissue coverage is insufficient.
Clinical use: Complex ridge augmentations and extensive reconstructive cases.
5-Choosing the Right Material
The selection of graft and membrane depends on:
- Defect size and morphology
- Patient’s systemic condition
- Desired resorption rate
- Surgical experience and handling preference
- Budget and material availability
Many clinicians use combinations, such as xenograft with a collagen membrane, to achieve both biological activity and long-term dimensional stability.
6-Clinical Applications in Implantology
- Socket preservation after extraction
- Sinus floor elevation (sinus lift)
- Ridge augmentation (horizontal and vertical)
- Peri-implant defect correction
- Periodontal regeneration
Each application requires a careful balance between biological integration and mechanical support, ensuring a predictable environment for implant placement.
7-The Future of Bone Regeneration
Modern research is focusing on biomimetic materials, stem cell therapy, and growth factor–enriched scaffolds (such as rhBMP-2 and PRF membranes) that can accelerate healing and improve bone quality.
3D-printed custom grafts and resorbable titanium meshes are also emerging as promising innovations in regenerative dentistry.
Conclusion
Bone grafts and membranes are the foundation of predictable implant success in modern dentistry. By understanding the properties, indications, and limitations of each material, clinicians can select the most suitable combination for every case — ensuring stable, esthetic, and long-lasting results.
Contact us today to learn how we can support your clinic with premium-quality implant regeneration products.
